Consensus Signal in Action
Learn how automated ADT notifications lead to improved patient care.
As of May 1, 2021, providers will require event notifications to be in place to follow the latest CMS ruling. Stay in compliance today and start delivering value.
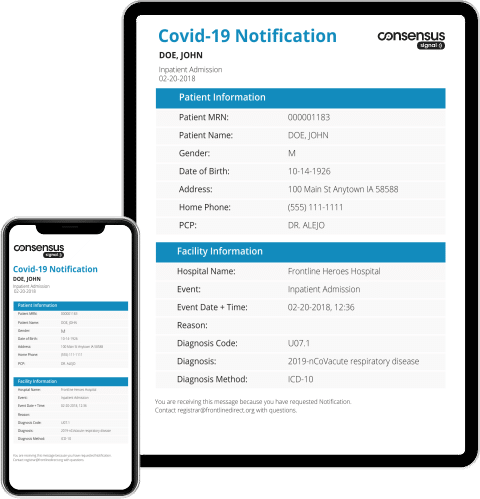
Consensus Signal delivers real-time health event alert notifications, connecting providers and care teams wherever patients receive care.
Consensus has joined with the leading event alerting solution in the market. Our partner, Secure Exchange Solutions, provides a nationwide reach into EHRs and access to nationwide directory services to easily find the provider for each patient. This means we deliver notifications directly into the workflow of receiving providers EHRs without requiring costly interfaces. No need to upload lists of patients or even have an EHR, we can deliver readable alerts into existing email clients

Communication gaps put patients at risk; an estimated 80% of serious medical errors involve miscommunication during
patient transfers or hand-offs.
Highlights
- Real-time alerts about patient admission, discharge and transfer for providers and care teams
- Coordinate care by sharing patient information and bridging gaps in patient history
- Manages COVID-19 Patient Activity
- Actionable data integrated into provider’s workflow improves decision-making
- Employ industry-standards like structured data that can be consumed by EHRs
- Effective follow-up within seven days of patient discharge
- Cost effective and easy to implement – no IT resources needed
- Keep doing what you do – no need to change your current workflows
- Rely on industry leader with years of focus in healthcare and a comprehensive solution suite
Real-time health event notifications let providers, care managers, and caregivers know when patients receive care, enabling better clinical decision-making and improved patient coordination.
What You Should Know About CMS Interoperability Rule
CMS New Conditions of Participation (CoPs)
Admission, Discharge, and Transfer (ADT) Event Notifications
Applicable May 1, 2021
The new Conditions of Participation (CoPs) require mandatory notification compliance for Medicare and Medicaid participating hospitals, including psychiatric hospitals and CAHs, to send electronic patient event notifications of patients’ admission, discharge, and/or transfer to their primary care provider.
Hospitals
“Electronic patient notifications are a proven tool for improving transitions of
care between settings and improving patient safety.”
CMS Interoperability and ONC Rule
Seema Verma, CMS Administrator

Who we serve:
-
Hospitals, Pharmacies, and Health Systems
Deliver automated ADT health alerts to meet CMS requirements, cut costs, reduce readmissions, and improve care.
-
Ambulatory Providers and Post-acute care organizations
Utilize alerts to enhance care coordination, speed authorizations and inform skilled nursing facilities, home health and assisted living.
-
Commercial Health Plans
Manage high risk members and close gaps in care integrated into EHR workflows to meet quality and costs measures and value-based care reimbursement.
-
Medicaid
Effectively manage high risk patients to improve transitions of care, enhance medical decision making and reduce costly and preventable readmissions.
-
90 Integrated EHR & Health Application Vendors
Plus 300+ EHRs in the Trust Community.






